Vitiligo is a skin condition that causes skin patches to lose color, making them appear lighter or white. It happens when the cells that produce skin color, called melanocytes, stop working or are destroyed.
Although there is no cure for vitiligo, treatments can help manage its appearance and slow its spread. This article will explain the causes, symptoms, and ways to treat and manage vitiligo, offering tips on how to care for your skin and reduce its impact.
Recommended Reading: Continuous Glucose Monitor Price In Pakistan [CGM Types, Uses, & Prices]
How To Prevent Vitiligo? Causes, Symptoms & Treatment

Table Of Contents
Recommended Reading: Top 10 Eye Drops For Red Eyes In Pakistan [Price, Uses, & Side Effects]
Causes of Vitiligo
Causes of Vitiligo
Vitiligo occurs when the immune system attacks melanocytes, the cells responsible for skin color. Common causes include:
- Genetic Factors: Family history increases the risk.
- Environmental Triggers: Sunburn, chemical exposure, and stress can accelerate its onset and spread.

What Causes Vitiligo?
Vitiligo happens when the body’s immune system attacks and destroys the cells that give skin its color, called melanocytes. Here are some common reasons why vitiligo may occur:
Genetic Factors
If someone in your family has vitiligo, you may be more likely to get it. Family history can play a role in causing this skin condition.
Environmental Triggers
Certain factors like getting a bad sunburn, being exposed to harmful chemicals, or going through high levels of stress can make vitiligo start or spread faster. These triggers can worsen the condition.
Recommended Reading: 5 Best Eye Drops For Infection In Pakistan
Symptoms of Vitiligo
Symptoms of Vitiligo
Vitiligo begins with small white patches on sun-exposed areas like the face, hands, or arms. Over time, these patches may grow and spread, with hair in affected areas turning gray or white. Those with a family history, frequent sunburns, or high stress should watch for early signs.
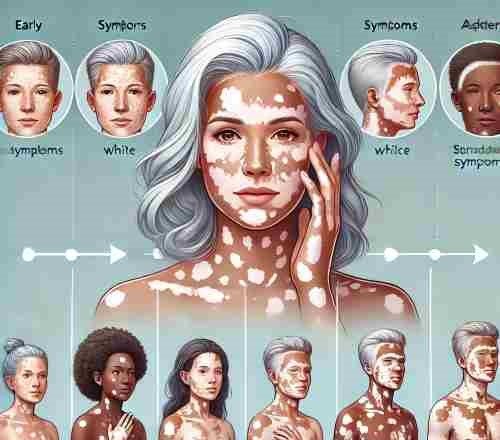
Early Symptoms
The first signs of vitiligo are usually white patches on the skin. These patches often appear on areas exposed to the sun, like the face, hands, or arms.
Advanced Symptoms
As vitiligo progresses, the white patches may grow larger and spread to other parts of the body. Hair in these affected areas may also turn gray or white.
Who Should Watch for Symptoms?
People with a family history of vitiligo should pay attention to any changes in their skin. Additionally, those who have frequent sunburns or experience high emotional stress may also be at risk.
Recommended Reading: Lavender Oil Uses For Hair | Lavender Essential Oil In Hair
How To Cure Vitiligo Permanently?
| Treatment Type | Description / Examples | Is it “permanent cure”? | Typical Repigmentation Success Rate (approx.) | Best For / Notes | Potential Drawbacks / Limitations |
|---|---|---|---|---|---|
| Topical JAK Inhibitors | Ruxolitinib cream (Opzelura) — FDA-approved | No | Face: ~30% achieve ≥75% at 6 months, ~50% at 1 year; body lower | Facial/non-segmental vitiligo; first targeted repigmentation therapy | Local side effects (acne, itching); expensive; relapse possible if stopped |
| Oral JAK Inhibitors | Upadacitinib (RINVOQ), others in trials/approval process | No | Significant repigmentation in phase 3 (e.g., T-VASI 50 achieved); details emerging | Widespread non-segmental; systemic option | Systemic risks (infections, lab changes); not yet universally approved for vitiligo |
| Phototherapy | Narrowband UVB (NB-UVB), 308 nm excimer laser | No | 50–75% in many patients (face/neck highest); ~70%+ with excimer in some studies | Widespread or facial/body; often combined with topicals | Time-intensive (2–3×/week); burns possible; maintenance needed; relapse common |
| Topical Corticosteroids / Calcineurin Inhibitors | Strong steroids, tacrolimus/pimecrolimus | No | 45–65% (face best); higher when combined | Limited areas, especially face/neck | Skin thinning (steroids), burning (tacrolimus); off-label for some |
| Surgical Options | Melanocyte transplantation, punch grafting, ReCell system | Closest to durable in stable cases | >75–90% in stable localized areas (some studies show long-term stability) | Stable vitiligo (no spread ≥1–2 years); small/segmental areas | Invasive; only for stable disease; risk of scarring/koebner; not for active spreading |
| Emerging / Experimental | Stem cell therapies, microbial compounds, IL-15 blockers, prostaglandin + UVB combos | No (still in trials) | Promising in early studies (e.g., 70%+ reduction in models); human data limited | Future hope for more durable repigmentation | Not widely available; mostly preclinical/early trials; years from routine use |
| Depigmentation | Monobenzone/hydroquinone to bleach remaining skin | Permanent color loss (not cure) | 70–90% uniform depigmentation | Very extensive vitiligo (>50% body); irreversible | Permanent; sun sensitivity; psychological impact; not repigmentation |
How To Prevent Vitiligo In Babies
| Approach / Measure | Description / How to Implement | Evidence Level & Effectiveness for Prevention in Babies | Key Notes & Limitations | Sources (2024–2026) |
|---|---|---|---|---|
| Strict Sun Protection | Use broad-spectrum sunscreen (SPF 30–50+), apply generously/reapply every 2 hours; dress in lightweight long sleeves, hats, seek shade; avoid peak sun hours (10 AM–4 PM). For infants <6 months: shade + clothing only (sunscreen not routinely recommended). | Highest — Most consistent trigger avoidance; sunburn strongly linked to onset/triggering. | Does NOT guarantee prevention (genetics dominate); protects depigmented areas from burns/cancer if vitiligo develops later. | AAD, Cleveland Clinic, Stanford, Kidsville Pediatrics, Medical News Today |
| Avoid Skin Trauma / Injury | Gentle handling; avoid harsh scrubbing, tight clothing friction, or unnecessary procedures on skin. | Moderate — Koebner phenomenon (new patches after injury) possible, though less common in infants. | Rare in babies; more relevant if vitiligo already present. | General vitiligo literature |
| Gentle Skin Care Routine | Use mild, fragrance-free soaps/cleansers; daily moisturizing to prevent dryness/irritation. Avoid harsh chemicals or known irritants. | Low to moderate — Reduces potential inflammatory triggers. | No direct proof it prevents onset; helps overall skin health. | Kidsville Pediatrics, general pediatric advice |
| Healthy Diet & Nutrition | Balanced infant nutrition (breast milk/formula, later varied solids); ensure adequate vitamin D (via diet/supplement if needed). Some suggest antioxidant-rich foods later. | Low — No strong evidence diet prevents vitiligo; vitamin D may support repigmentation if disease occurs. | No proven preventive diet; unproven claims (e.g., excess water, specific herbs) lack evidence. | Stanford Children’s, Vitiligo Society |
| Stress Reduction (for family) | Calm environment; minimize family stress (though hard to quantify in babies). | Low — Stress is a reported trigger in older children/adults, less clear in infants. | Not practical/measureable in newborns; indirect benefit. | General vitiligo triggers |
| Avoid Chemical Exposures | Limit unnecessary exposure to phenols/chemicals (e.g., in some adhesives, dyes); use baby-safe products. | Low — Rare occupational-type triggers in adults; negligible in babies. | Not a realistic concern for most infants. | Older literature |
| Genetic Counseling (if family history) | Consult geneticist/dermatologist if strong family history of vitiligo/autoimmune diseases. | Informational only — Risk to child ~5–6% even with parent affected; no intervention changes genes. | Helps set expectations; no preventive treatment. | Recent genetic studies (2025) |
| Unproven / Ineffective Methods | Special diets (gluten-free, etc.), supplements, herbs, “immune boosters,” avoiding vaccines (no link), etc. | None — No scientific support for prevention. | Can delay real care or cause harm; avoid misinformation. | AAD, Mayo Clinic, NIH sources |
How To Prevent Vitiligo In Kids
| Approach / Measure | How to Implement in Children | Evidence Level & Potential Benefit for Prevention | Key Notes & Realistic Expectations | Supporting Sources (Recent) |
|---|---|---|---|---|
| Rigorous Sun Protection | Use broad-spectrum SPF 50+ sunscreen (apply generously, reapply every 2 hours); dress in lightweight long sleeves, pants, wide-brimmed hats; seek shade; avoid peak sun (10 AM–4 PM). For babies <6 months: mainly shade/clothing (sunscreen if needed, per pediatrician). | Highest — Severe sunburn is one of the most consistently linked triggers for onset or new patches. | Does not guarantee prevention (genetics primary); protects depigmented skin if vitiligo develops; reduces skin cancer risk long-term. | AAD, Cleveland Clinic, Stanford Children’s, NHS, AAP Pediatric Education |
| Avoid Skin Trauma / Injury (Koebner Phenomenon) | Gentle handling; avoid rough play leading to cuts/scrapes/burns; protect during sports/activities; treat wounds promptly with gentle care; avoid harsh scrubbing or tight/friction clothing. | Moderate — Skin injury can trigger new patches in predisposed kids. | More relevant once vitiligo starts, but minimizing unnecessary trauma is low-risk advice. | AAD, Cleveland Clinic, general vitiligo literature |
| Gentle Skin Care Routine | Use mild, fragrance-free soaps/cleansers; moisturize daily with gentle, unscented products to prevent dryness/irritation; avoid harsh chemicals/irritants. | Low to moderate — Reduces potential inflammatory or irritant triggers. | Supports overall skin health; no direct proof for preventing onset. | Stanford Children’s, Kidsville Pediatrics, general pediatric dermatology |
| Healthy Balanced Diet & Nutrition | Encourage varied, nutritious foods (fruits, vegetables, whole grains); ensure adequate vitamin D (via diet, safe sun, or supplement if deficient — check with doctor); focus on antioxidants/anti-inflammatory foods. | Low — No strong evidence specific diets prevent onset; vitamin D may support if disease occurs. | Avoid unproven restrictive diets (e.g., extreme gluten-free without testing); no “magic” foods cure/prevent. | Stanford Children’s, Vitiligo Society, recent reviews |
| Stress Management | Create calm environment; encourage play, good sleep, family routines; teach simple relaxation (e.g., breathing for older kids); minimize chronic family stress. | Low — Stress reported as trigger in some cases (more in older kids/adults); less clear in young children. | Indirect benefit for overall well-being; hard to quantify in toddlers. | AAD, MyVitiligoTeam, general triggers |
| Avoid Unnecessary Chemical Exposures | Use baby/child-safe products; limit exposure to strong chemicals (e.g., certain dyes, phenols in some items). | Low — Rare in kids; more adult occupational. | Not a major concern for most children. | Older literature, NHS triggers |
| Genetic Counseling / Monitoring (if strong family history) | Consult pediatric dermatologist or geneticist if parent/sibling has vitiligo/autoimmune diseases. | Informational — Risk to child ~5–25% with affected parent; no gene-editing available. | Helps early detection/monitoring; no preventive drug exists. | Recent genetic/autoimmune studies |
| Unproven / Not Recommended Methods | Special “anti-vitiligo” diets, excess supplements/herbs, avoiding vaccines (no link), etc. | None — Lack scientific support; can be harmful or delay care. | Avoid misinformation; focus on proven steps. | AAD, Mayo Clinic, Cleveland Clinic |
How to Prevent Vitiligo
How to Prevent Vitiligo
While vitiligo can’t be cured, prevention strategies can slow its spread. Protect your skin with sunscreen, wear protective clothing, and follow a healthy diet rich in anti-inflammatory foods. Vitamins D, C, and E support skin health, while stress management through meditation or yoga helps prevent flare-ups.

Prevention Strategies
Although vitiligo cannot be completely cured, some steps may help slow down its spread and protect your skin.
Sun Protection
It’s important to protect your skin from the sun. Use sunscreen with an SPF of 30 or more, wear protective clothing, and try to stay in the shade during the hottest parts of the day.
Healthy Diet
Eating healthy can help. Avoid foods that cause inflammation, like processed meats and sugary snacks. Instead, eat more leafy greens, berries, and fish, which have anti-inflammatory benefits.
Vitamins and Supplements
Adding vitamins like D, C, and E to your diet can help boost your immune system and protect your skin.
Managing Emotional Stress
Stress can make vitiligo worse, so it’s important to manage it. Practices like meditation or yoga can help reduce stress levels and support overall well-being.
Recommended Reading: Postpartum Depression Treatment At Home [Naturally]
Treatment Options for Vitiligo
Topical Medications
Creams such as corticosteroids and tacrolimus ointment can be applied to the skin to help restore color in affected areas.
Light Therapy
UVB light therapy is a treatment that uses special light to encourage the production of melanocytes, the cells that give your skin its color.
Surgical Treatments
For more severe cases, surgeries like skin grafts or melanocyte transplantation can be options to restore color to larger areas of the skin.
Camouflage Therapies
Special makeup products are available to cover up white patches, helping to improve appearance for cosmetic reasons.
Oral Medications
In some cases, doctors may prescribe medications that suppress the immune system to slow down the spread of vitiligo.
Recommended Reading: Vaginal Dryness Natural Remedies [Symptoms & Treatments]
How To Avoid Vitiligo From Spreading
- Seek prompt medical treatment for active/progressive vitiligo — The #1 way to halt spread is starting evidence-based therapy early. Options include:
- Topical JAK inhibitors (e.g., ruxolitinib/Opzelura cream) — Often first-line for many; helps stop progression and repigment.
- Topical corticosteroids or calcineurin inhibitors (tacrolimus/pimecrolimus) — Frequently stop spread in limited areas, especially when used early.
- Narrowband UVB phototherapy (NB-UVB) — Proven to slow or stop progression in active disease; often combined with topicals for better results.
- Oral JAK inhibitors (e.g., upadacitinib/RINVOQ — recent approvals/submissions in 2026) or short courses of oral corticosteroids (e.g., mini-pulse therapy) — Used for rapidly spreading or widespread cases to quickly stabilize.
- Protect your skin rigorously from sunburn and excessive sun exposure — Severe sunburn is one of the most common and powerful triggers for new patches or faster spread.
- Apply broad-spectrum sunscreen (SPF 50+ PA++++, water-resistant) to all exposed skin daily — reapply every 2 hours outdoors.
- Wear protective clothing (long sleeves, wide-brimmed hats, UPF clothing), seek shade, avoid peak sun hours (10 AM–4 PM).
- Depigmented skin burns very easily and increases skin cancer risk long-term.
- Avoid or minimize skin trauma and injury (Koebner phenomenon) — New white patches often appear at sites of cuts, burns, friction, scrapes, or irritation.
- Handle skin gently; avoid harsh scrubbing, tight clothing/belts that rub, or unnecessary skin procedures.
- Protect skin during sports/activities; treat any wounds promptly and gently.
- Avoid harsh chemicals, strong exfoliants, or unnecessary adhesives on skin.
- Manage stress effectively — Emotional or physical stress is a frequently reported trigger that can accelerate autoimmune activity and spread.
- Practice relaxation techniques (meditation, yoga, deep breathing, mindfulness).
- Maintain good sleep, exercise regularly, and seek support (counseling if needed).
- Reduce chronic stressors where possible.
- Follow a gentle, consistent skincare routine — Prevent irritation, dryness, or inflammation that could indirectly contribute.
- Use mild, fragrance-free cleansers and daily moisturizers.
- Avoid abrasive scrubs, hot showers, or known irritants.
- Consider maintenance therapy after stabilization — Once spread stops and some repigmentation occurs, ongoing low-intensity treatment helps prevent relapse.
- Intermittent topical meds, periodic phototherapy sessions, or low-dose maintenance as prescribed.
- Monitor closely and act fast on changes — Track patches with photos; see your dermatologist immediately if new spots appear or existing ones enlarge — early treatment is far more effective at stopping progression.
Pros & Cons of Vitiligo Treatments
Advantages
- Topical Treatments: These creams are helpful in the early stages of vitiligo and can restore skin color over time.
- Light Therapy: This treatment encourages pigment production, helping to bring color back to the skin.
- Surgery: For some people, surgery can provide long-lasting results by restoring color to large areas.
Disadvantages
- Topical Treatments: Some creams can cause side effects like skin thinning, especially with long-term use.
- Light Therapy: It requires regular treatments for several months and may take time to show results.
- Surgery: It isn’t suitable for everyone and comes with potential risks, like infection or scarring.
Recommended Reading: 11 Best Essential Oils In Pakistan (100% Pure & Natural)
FAQs
What is vitiligo?
Vitiligo is a skin condition where white patches appear because the skin loses its color. This happens when the cells that make pigments are damaged or destroyed.
Is vitiligo contagious?
No, vitiligo is not contagious. It cannot spread from person to person through contact.
What causes vitiligo?
Vitiligo is believed to be caused by the immune system mistakenly attacking the cells that produce skin color. Other factors like genetics, sunburn, or stress might also play a role.
Can vitiligo be cured?
There is no cure for vitiligo, but treatments can help restore some color to the skin and manage the condition.
What treatments are available for vitiligo?
Treatments include topical creams, light therapy, surgery, and camouflage makeup to cover the white patches.
Can diet help with vitiligo?
While there’s no special diet to cure vitiligo, a healthy diet rich in vitamins like C, D, and E can support immune health and overall skin health.
How can I prevent vitiligo from getting worse?
You can protect your skin by using sunscreen, avoiding sunburn, managing stress, and following a healthy lifestyle to help prevent vitiligo from worsening.
Can vitiligo spread to other parts of the body?
Yes, in some cases, vitiligo may spread to other parts of the body over time, but the rate at which it spreads varies from person to person.
Conclusion
Recommended Reading: 10 Best Medicine For Anxiety And Depression In Pakistan
Summary of Key Points
Vitiligo is a condition where the skin loses color, and although there is no cure, the symptoms can be controlled. Sun protection, a healthy diet, and proper medical treatments can help manage it.
Who Should Take Action?
If you notice early signs of vitiligo, like white patches on your skin, it’s important to consult a doctor quickly. Early action can help stop the condition from getting worse.
Final Thoughts
Managing vitiligo requires a mix of preventive care, medical treatments, and healthy lifestyle choices. With the right plan, people with vitiligo can live better and manage their symptoms effectively.
Disclaimer
Commissions we earn from partner links on this page do not influence our content. Our editorial content is based on thorough research and insights from qualified medical professionals to ensure the highest standards of accuracy and reliability.
Information provided on Doseway is for educational purposes only. Your health and wellness are unique to you, and the products and services we review may not be suitable for your individual circumstances. We do not offer personal medical advice, diagnosis, or treatment plans. For specific advice, please consult with a healthcare professional. Doseway adheres to strict editorial integrity standards. To the best of our knowledge, all content is accurate as of the date posted, though offers and information may change. The opinions expressed are the author’s own and have not been influenced, approved, or endorsed by our partners.

 Cart is empty
Cart is empty
Add a Comment