Psoriasis with psoriatic arthritis is a condition that affects both the skin and the joints. Psoriasis causes red, scaly patches on the skin, while psoriatic arthritis leads to joint pain, stiffness, and swelling. These two conditions often occur together, and they can cause significant discomfort and affect your daily life.
Psoriatic arthritis can impact various joints, including the fingers, toes, spine, and even the hips. While there is no cure for these conditions, treatments are available to help manage symptoms, reduce inflammation, and improve quality of life.
Recommended Reading: New Type 2 Diabetes Treatments (Causes+Symptoms)
Psoriasis With Psoriatic Arthritis – Symptoms Causes, And Treatment

Table Of Contents
Recommended Reading: Top 7 Epilepsy Treatment Medicine | Anti-Seizure Drugs List
Psoriasis with Psoriatic Arthritis
Psoriasis with Psoriatic Arthritis
Psoriatic arthritis is an autoimmune condition affecting both skin and joints, causing inflammation, pain, swelling, and stiffness. It often impacts the fingers, toes, spine, and other joints, along with red, scaly skin patches. Symptoms include joint pain, nail changes, eye inflammation, and fatigue.
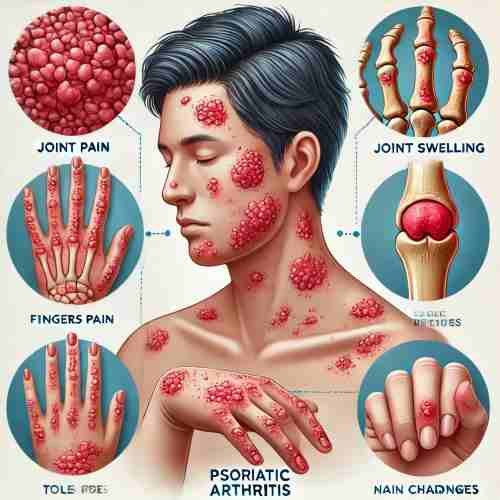
What is Psoriatic Arthritis?
Psoriatic arthritis is a type of autoimmune condition that impacts both the skin and the joints. It causes inflammation in the joints, leading to pain, swelling, and stiffness, while also causing skin rashes similar to those seen in psoriasis. This condition often affects areas such as the spine, fingers, and toes, and can make everyday tasks difficult due to discomfort and reduced mobility.
How Does Psoriatic Arthritis Affect the Body?
In psoriatic arthritis, the immune system mistakenly attacks healthy tissues in the joints, causing swelling, pain, and sometimes damage over time. On the skin, it leads to red, scaly patches commonly found on the scalp, elbows, or knees. Joint pain is a hallmark of the condition and can occur in areas like the fingers and toes, often making movement painful and challenging.
Recommended Reading: Top 5 Symptoms Of Piles In Females (Symptoms & Cure)
What Are The 5 Types Of Psoriatic Arthritis
| Type | Key Characteristics | Affected Areas | Prevalence | Symptoms and Details |
|---|---|---|---|---|
| Asymmetric Oligoarthritis | Involves fewer than 5 joints, typically on one side of the body (asymmetric). | Knees, ankles, wrists, or fingers/toes (dactylitis common). | Most common type (about 35-50% of PsA cases). | This is often the mildest form and the initial presentation for many patients. It causes swelling, pain, and stiffness in a few joints, not mirroring on both sides. Dactylitis (sausage-like swelling of digits) and enthesitis (inflammation at tendon insertions) are frequent. It may progress to other types if untreated. Skin psoriasis may precede or coincide with joint symptoms. |
| Symmetric Polyarthritis | Involves 5 or more joints symmetrically on both sides of the body, resembling rheumatoid arthritis. | Small joints of hands and feet, wrists, ankles, and sometimes larger joints like knees or elbows. | Common (about 25-40% of cases). | This type mimics rheumatoid arthritis but is seronegative (no rheumatoid factor). Patients experience widespread joint pain, swelling, morning stiffness lasting over an hour, and fatigue. Nail changes (pitting, onycholysis) are common. It can lead to joint deformities if progressive, and extra-articular features like eye inflammation (uveitis) may occur. |
| Distal Interphalangeal Predominant (DIP) | Primarily affects the distal interphalangeal joints (fingertips). | DIP joints of fingers and toes; may involve nails heavily. | Less common (about 5-15% of cases). | Characterized by inflammation at the ends of fingers/toes, often with severe nail involvement (e.g., crumbling or separation). It can cause “pencil-in-cup” deformities on X-rays. Pain and swelling are localized but can be debilitating for fine motor tasks. This type is strongly linked to psoriasis and may overlap with other forms. |
| Spondylitis (Axial PsA) | Involves the spine and sacroiliac joints, similar to ankylosing spondylitis. | Spine (neck, back), sacroiliac joints; may extend to peripheral joints. | About 15-25% of cases; more common in men. | Focuses on axial skeleton, causing back pain, stiffness (worse in the morning or after inactivity), and reduced spinal mobility. It can lead to fusion of vertebrae (ankylosis) over time. Peripheral symptoms like enthesitis or dactylitis may coexist. HLA-B27 gene is often positive. Eye involvement (uveitis) is more frequent here. |
| Arthritis Mutilans | Severe, deforming type with bone resorption and joint destruction. | Fingers, toes, and sometimes other joints; leads to telescoping digits. | Rare (about 5% of cases); most destructive form. | Known as the “opera glass” or telescoping finger deformity due to bone dissolution (osteolysis). It causes severe pain, instability, and disability. Joints become floppy and shortened. This type often requires aggressive treatment to prevent progression, and it’s associated with long-standing, untreated PsA. |
Psoriatic Arthritis Treatment
- Mild symptoms — Start with symptomatic relief.
- Moderate to severe or progressive — Move quickly to disease-modifying therapies (DMARDs), often biologics or targeted synthetics early (per EULAR 2023 and recent data favoring IL-17/IL-23 pathways).
- Skin-dominant — Prioritize agents effective for both (e.g., IL-17 or IL-23 inhibitors).
| Category | Examples (Common/Top in 2025) | Key Benefits | Best For | Notes / Recent Highlights |
|---|---|---|---|---|
| NSAIDs | Ibuprofen, naproxen, celecoxib | Quick pain/swelling relief | Mild, short-term use | Limited role now; max 4 weeks monotherapy in mild cases (EULAR). Not disease-modifying. |
| Conventional synthetic DMARDs (csDMARDs) | Methotrexate (most common), leflunomide, sulfasalazine | Slow disease progression, joint protection, some skin benefit | Moderate peripheral arthritis; often first systemic step | Methotrexate remains widely used; monitor liver/blood counts. Less favored as first-line in severe cases. |
| TNF inhibitors (TNFi biologics) | Adalimumab (Humira), etanercept (Enbrel), infliximab, certolizumab, golimumab | Excellent for joints, enthesitis, dactylitis, axial, and skin; prevent damage | First-line biologic in many guidelines (ACR/NPF); treatment-naïve active PsA | Still strong option; biosimilars make them more accessible/affordable. |
| IL-17 inhibitors | Secukinumab (Cosentyx), ixekizumab (Taltz), bimekizumab (Bimzelx) | Superior skin clearance + strong joint efficacy; good for enthesitis/dactylitis | Moderate-severe skin + joints; axial disease | IL-17/IL-23 pathway cornerstone; bimekizumab (dual IL-17A/F) highly effective for skin/joints. |
| IL-23 inhibitors | Guselkumab (Tremfya), risankizumab (Skyrizi), ustekinumab (Stelara; IL-12/23) | Excellent long-term skin control; joint efficacy; guselkumab slows radiographic progression | Skin-dominant or joint preservation | Guselkumab first IL-23 to show structural damage inhibition in PsA (2025 data). |
| JAK inhibitors (tsDMARDs) | Upadacitinib (Rinvoq), tofacitinib (Xeljanz), deucravacitinib (Sotyktu; TYK2) | Oral convenience; good for joints/skin; after TNFi failure in some cases | Oral preference; peripheral arthritis | Upadacitinib strong post-TNFi; deucravacitinib emerging oral for psoriasis/PsA. Safety monitoring (infections, CV, etc.) required. |
| PDE4 inhibitor | Apremilast (Otezla) | Oral; mild-moderate; some skin/joint benefit | Mild-moderate; intolerant to others | Lower efficacy than biologics; fewer side effects. |
| Other / Emerging | Abatacept (Orencia), sonelokimab (nanobody, in trials), others in development | Targeted options | Refractory cases | Sonelokimab promising in 2025 trials for rapid joint/skin improvement. |
Top 10 Best Medication For Psoriatic Arthritis
| Medicine (Brand Name Example) | Class / Mechanism | Administration | Key Strengths for PsA + Psoriasis | Common Use / Notes (2025-2026) |
|---|---|---|---|---|
| Guselkumab (Tremfya) | IL-23 inhibitor | Subcutaneous injection (every 4-8 weeks after loading) | Excellent skin clearance; strong joint efficacy; first IL-23 to slow radiographic joint damage progression (APEX trial 2025) | Top choice for skin-dominant or joint preservation; long-term data strong; pediatric approval expanded. |
| Secukinumab (Cosentyx) | IL-17A inhibitor | Subcutaneous injection (monthly maintenance) | Superior for enthesitis/dactylitis; very good skin + joint control; axial disease effective | Cornerstone IL-17 option; widely used first-line biologic in many cases. |
| Ixekizumab (Taltz) | IL-17A inhibitor | Subcutaneous injection (every 4 weeks) | Rapid, high skin clearance (PASI 90/100); strong peripheral joint response | Excellent for moderate-severe skin + joints; similar to secukinumab but dosing differences. |
| Adalimumab (Humira / biosimilars) | TNF inhibitor | Subcutaneous injection (every 2 weeks) | Proven long-term joint protection; good for all PsA domains (skin, axial, enthesitis) | Still a go-to first biologic; biosimilars improve affordability/access in places like Pakistan. |
| Etanercept (Enbrel / biosimilars) | TNF inhibitor | Subcutaneous injection (weekly) | Reliable for joints and skin; long safety track record | Common starter biologic; widely available. |
| Upadacitinib (Rinvoq) | JAK inhibitor | Oral tablet (daily) | Convenient oral; effective post-TNFi failure; good for peripheral arthritis/skin | Rising oral preference; monitor for infections/CV risks per guidelines. |
| Bimekizumab (Bimzelx) | Dual IL-17A/F inhibitor | Subcutaneous injection (every 4-8 weeks) | Potentially highest skin clearance; strong joint data (long-term BE OPTIMAL/COMPLETE studies) | Emerging top performer; gaining traction for refractory cases. |
| Risankizumab (Skyrizi) | IL-23 inhibitor | Subcutaneous injection (every 12 weeks maintenance) | Outstanding long-term skin control (high PASI 90 sustained); solid PsA efficacy | Great for maintenance; less frequent dosing. |
| Ustekinumab (Stelara) | IL-12/23 inhibitor | Subcutaneous injection (every 12 weeks) | Balanced skin/joint benefit; convenient dosing | Established option; good for patients with comorbidities. |
| Methotrexate (various generics) | Conventional DMARD | Oral tablet or injection (weekly) | Affordable; slows progression in peripheral arthritis; some skin benefit | Often first systemic (or combo with biologics); monitor liver/blood; still widely used globally/Pakistan. |
Symptoms of Psoriasis with Psoriatic Arthritis
Psoriasis with psoriatic arthritis can cause a combination of skin and joint symptoms. Commonly, it leads to pain, swelling, and stiffness in the joints, especially in the fingers, toes, and spine. Skin rashes resembling psoriasis may develop on areas such as the scalp, elbows, and knees.
Additionally, changes in the nails, like pitting (small dents) or crumbling, are common. Eye inflammation can also occur, causing redness, pain, or blurry vision.
Key Symptoms
- Joint pain, swelling, and stiffness, particularly in fingers, toes, and spine.
- Skin rashes resembling psoriasis on the scalp, elbows, or knees.
- Nail changes, such as pitting or crumbling.
- Eye inflammation leading to redness, pain, or blurry vision.
- Tenderness in areas where tendons or ligaments attach to bones.
- General tiredness or feeling unwell.
Causes and Risk Factors
Causes, Risk Factors and Treatment
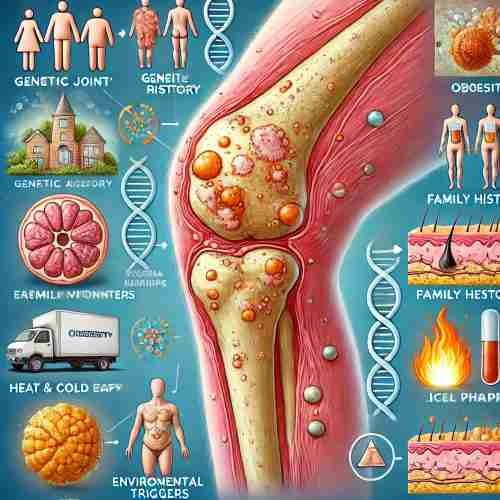
Psoriatic arthritis occurs when genetic and environmental factors trigger the immune system to attack the skin and joints, causing inflammation. Risk factors include obesity, family history, and severe psoriasis. Treatment options include NSAIDs, DMARDs, biologics, corticosteroids, heat and cold therapy, physical therapy, and lifestyle changes like yoga and weight management.
Recommended Reading: How To Relieve Constipation On The Toilet Immediately (Naturally)
What Causes Psoriasis with Psoriatic Arthritis?
Psoriatic arthritis develops when a mix of genetic and environmental factors trigger the immune system to attack healthy tissues, particularly in the joints and skin. If you already have psoriasis, you’re at a higher risk of also developing psoriatic arthritis. The condition occurs when the body’s immune system mistakenly attacks the skin and joints, leading to inflammation and discomfort.
Risk Factors
- Obesity: Carrying extra weight can increase the risk of joint problems, especially in people who already have severe psoriasis.
- Family History: If other family members have psoriasis or arthritis, your chances of developing psoriatic arthritis may be higher.
- Severe Psoriasis: People with more widespread psoriasis, especially those with large areas of the skin affected, are more likely to experience joint complications.
Treatment for Psoriatic Arthritis
Recommended Reading: Top 5 Constipation Relief Medicines For Babies
Medications
- NSAIDs (Nonsteroidal Anti-inflammatory Drugs): These are commonly used to help reduce pain and swelling. Examples include ibuprofen and naproxen.
- DMARDs (Disease-modifying Antirheumatic Drugs): These drugs, like methotrexate, are used to slow the progression of the disease and prevent further joint damage.
- Biologic Therapies: If DMARDs don’t work, biologics can target specific parts of the immune system to control inflammation and joint damage.
- Corticosteroids: These can be used for quick relief of inflammation and pain, typically for short periods.
Self-care
- Heat Therapy: Using heat wraps or warm baths can help reduce stiffness and ease muscle spasms.
- Cold Therapy: Applying cold packs to affected areas can help reduce swelling and soothe discomfort.
Physical Therapy
Engaging in low-impact activities like walking, swimming, or gentle yoga can improve joint mobility and ease stiffness.
Lifestyle Changes
- Modified Yoga and Pilates: These exercises can help improve flexibility and strengthen muscles around the joints.
- Healthy Weight and Activity: Maintaining a healthy weight and staying active can ease symptoms and help with overall well-being.
Effectiveness of Psoriatic Arthritis Treatments
Recommended Reading: Alternative Medicine For Joint Pain (Knee Pain Treatment)
Clinical Evidence
Research has shown that diagnosing psoriatic arthritis early and starting treatment with medications like DMARDs, NSAIDs, and biologics can significantly help manage symptoms. These treatments are proven to control pain, reduce inflammation, and prevent further damage to the joints over time.
Expected Results
The results of treatment can vary from person to person. However, with the right combination of medications and therapies, many people find that joint pain and skin rashes become more manageable. This often leads to a better quality of life, with less discomfort and improved mobility.
Recommended Reading: Stomach Acidity Medicine (Medicine For Acidity & Gas)
Side Effects & Precautions
Side Effects & Precautions
Psoriatic arthritis treatments can relieve pain, reduce swelling, and improve mobility, but they may cause side effects like indigestion (NSAIDs), dizziness, or increased infection risk (biologics). Serious risks include allergic reactions and osteoporosis from long-term corticosteroid use.
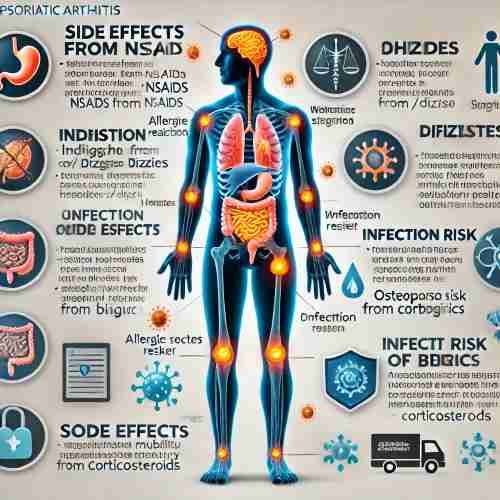
Common Side Effects
- NSAIDs may cause stomach problems like indigestion.
- Possible headaches or dizziness with pain-relief medications.
- Biologic therapies may increase the risk of infections due to their effect on the immune system.
Serious Side Effects
- Severe allergic reactions, including swelling or difficulty breathing.
- Long-term use of corticosteroids may weaken bones, increasing the risk of osteoporosis.
Precautions
- Discuss your medical history with your healthcare provider before starting treatment.
- Be aware of potential drug interactions that could worsen your condition or interfere with treatment.
Pros & Cons of Psoriatic Arthritis Treatments
Recommended Reading: Over The Counter Asthma Tablets (Best Medicine For Asthma Cough)
Advantages
Proper treatments for psoriatic arthritis, such as medications and lifestyle changes, can significantly reduce pain, swelling, and skin symptoms. They help improve joint mobility and overall quality of life, allowing you to move more freely and feel better day by day.
Disadvantages
Some treatments may come with side effects that can impact your overall health, such as stomach issues or an increased risk of infections.
Psoriatic arthritis can be tough to manage, but with the right treatments and lifestyle changes, symptoms can be controlled. While there is no cure, medications like NSAIDs, DMARDs, and biologics can help reduce pain, swelling, and skin issues, improving quality of life.
Who Should Use It
Anyone experiencing both psoriasis and joint pain should consider seeing a rheumatologist for personalized care. Early treatment is key to managing symptoms effectively.
Alternative Options
If medications don’t work as expected, alternatives such as physical therapy, self-care practices like heat or cold treatment, and lifestyle changes might offer relief and help manage the condition better.
Recommended Reading: Alternative Medicine For Knee Pain Treatment
FAQs
What is psoriatic arthritis?
Psoriatic arthritis is an autoimmune condition that affects both the skin and the joints. It typically causes joint pain, swelling, and stiffness, along with skin rashes similar to those of psoriasis. It can impact the joints in the fingers, toes, spine, and other areas.
What causes psoriatic arthritis?
Psoriatic arthritis is believed to be caused by a mix of genetic and environmental factors. If you have psoriasis, you are at a higher risk of developing psoriatic arthritis. Other factors like family history, obesity, and severe psoriasis may also increase your chances.
How do I know if I have psoriatic arthritis?
Common signs of psoriatic arthritis include joint pain, swelling, and stiffness, especially in the fingers and toes. You might also experience skin rashes, changes in nails, and eye inflammation.
Can psoriatic arthritis be cured?
There is no cure for psoriatic arthritis, but symptoms can be managed effectively with treatments such as medications, physical therapy, and lifestyle changes.
What treatments are available for psoriatic arthritis?
Treatment options include NSAIDs (for pain relief), DMARDs (to slow the disease’s progression), biologic drugs (for severe cases), and corticosteroids (to reduce inflammation). Self-care techniques like heat/cold therapy and exercises can also help manage symptoms.
Can lifestyle changes help with psoriatic arthritis?
Yes, maintaining a healthy weight, staying active, and doing low-impact exercises such as swimming or yoga can help improve joint mobility and reduce pain.
Recommended Reading: Top 5 Constipation Relief Medicines For Babies
Disclaimer
Commissions we earn from partner links on this page do not influence our content. Our editorial content is based on thorough research and insights from qualified medical professionals to ensure the highest standards of accuracy and reliability.
Information provided on Doseway is for educational purposes only. Your health and wellness are unique to you, and the products and services we review may not be suitable for your circumstances. We do not offer personal medical advice, diagnosis, or treatment plans. For specific advice, please consult with a healthcare professional. Doseway adheres to strict editorial integrity standards. To the best of our knowledge, all content is accurate as of the date posted, though offers and information may change. The opinions expressed are the author’s own and have not been influenced, approved, or endorsed by our partners.

 Cart is empty
Cart is empty
Add a Comment